
What if I am wearing my monitor and I don’t have any symptoms?ĭetecting an arrhythmia is much like fishing. The advantage of wireless cloud based technology, is patients can be alerted in real time of any dangerous rhythm abnormalities. The information is either stored directly onto a hard drive, and downloaded in the doctor’s office for interpretation, or transmitted wirelessly to a cloud. Wires typically transmit this, however newer monitors can now work via wireless technology. Event monitors only record activity when triggered by the patient when symptoms occur.Įlectrodes are placed on the skin, and transmit ECG information to a storage device. They provide continuous monitoring of a persons electrical heart activity (ECG). Holter monitors can be worn for 24-48 hours, or even extended periods of time. 
The two basic types of monitors are holter monitors and event monitors. What are the different types of heart monitors? Heart monitors are extremely useful tools that doctors use to accurately make a diagnosis. Examples of medical diagnoses are atrial fibrillation, premature ventricular contractions, and premature atrial contractions. Palpitations and Dizziness are NOT medical diagnoses. The most important decisions a doctor can make are predicated on having an accurate diagnosis. An ambulatory heart monitor typically has 3-6 electrodes attached to the skin, that provides information to a storage device or cloud that can be more sensitive in making a diagnosis. Often, 10 seconds isn’t enough time to make a diagnosis, so an ambulatory heart monitor is ordered. An ECG has 12 electrodes attached to the skin that transmit electrical signals from the heart for 10 seconds. First patients are screened with an ECG (electrocardiogram). Heart monitors are vital in making a diagnosis. Patients presenting with dizzy symptoms often need cardiac evaluation, to determine if low heart rates or high heart rates are responsible for their symptoms. It is very important to have a diagnosis to delineate the more serious forms of palpitations from the more benign variety. Occasionally palpitations can be associated with serious underlying heart conditions. Most palpitations are not serious, and more of a nuisance. 
Palpitations are any symptoms of extra hard beats, skipped beats, or heart fluttering. One of the most common symptoms patients complain of is palpitations. Patients experiencing any cardiac symptoms should consult a physician. Once a diagnosis is made, patients can be offered therapy to help with symptoms. Routine periodic ischaemic evaluations with stress echocardiography or myocardial perfusion studies are controversial.My job as a cardiologist is to help make a diagnosis when symptoms arise. 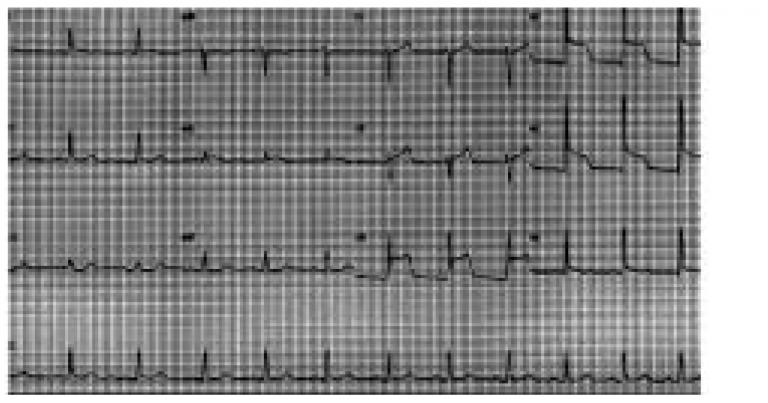
They should be evaluated by stress testing or cardiac catheterisation if symptoms develop. Patients with a history of MI are at increased risk for recurrent infarction. Patients who develop diminished LV function and congestive heart failure should be followed up and managed appropriately. Patients with ejection fraction <35% at 3 months' follow-up should be referred to an electrophysiologist for consideration of an implantable cardioverter defibrillator (ICD), as there is a high risk for arrhythmias in this population. This includes dual antiplatelet therapy with aspirin plus ticagrelor, prasugrel, or clopidogrel (for at least 1 year) beta-blockers statins and ACE inhibitors (especially in patients with decreased ejection fraction).Įjection fraction is assessed by echocardiography during the index hospital admission, possibly 3 months after the acute episode (depending on physician discretion and/or institutional protocols) and then periodically thereafter, depending on left ventricular (LV) function and symptoms. All patients should continue the optimal medical regimen indefinitely. Initiating risk-factor modification and aggressive medical management prior to discharge has been associated with increased patient adherence. Patients should be evaluated within 2 to 3 weeks of discharge and evaluated periodically based on the extent of myocardial damage and patient condition. Survivors of acute MI should be closely followed up to ensure adequate modification of risk factors and optimisation of (and adherence to) pharmacotherapy for secondary prevention, as well as to monitor for the development of post MI complications and/or residual angina symptoms.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
